Doxycycline for Strep Throat: Does It Work?
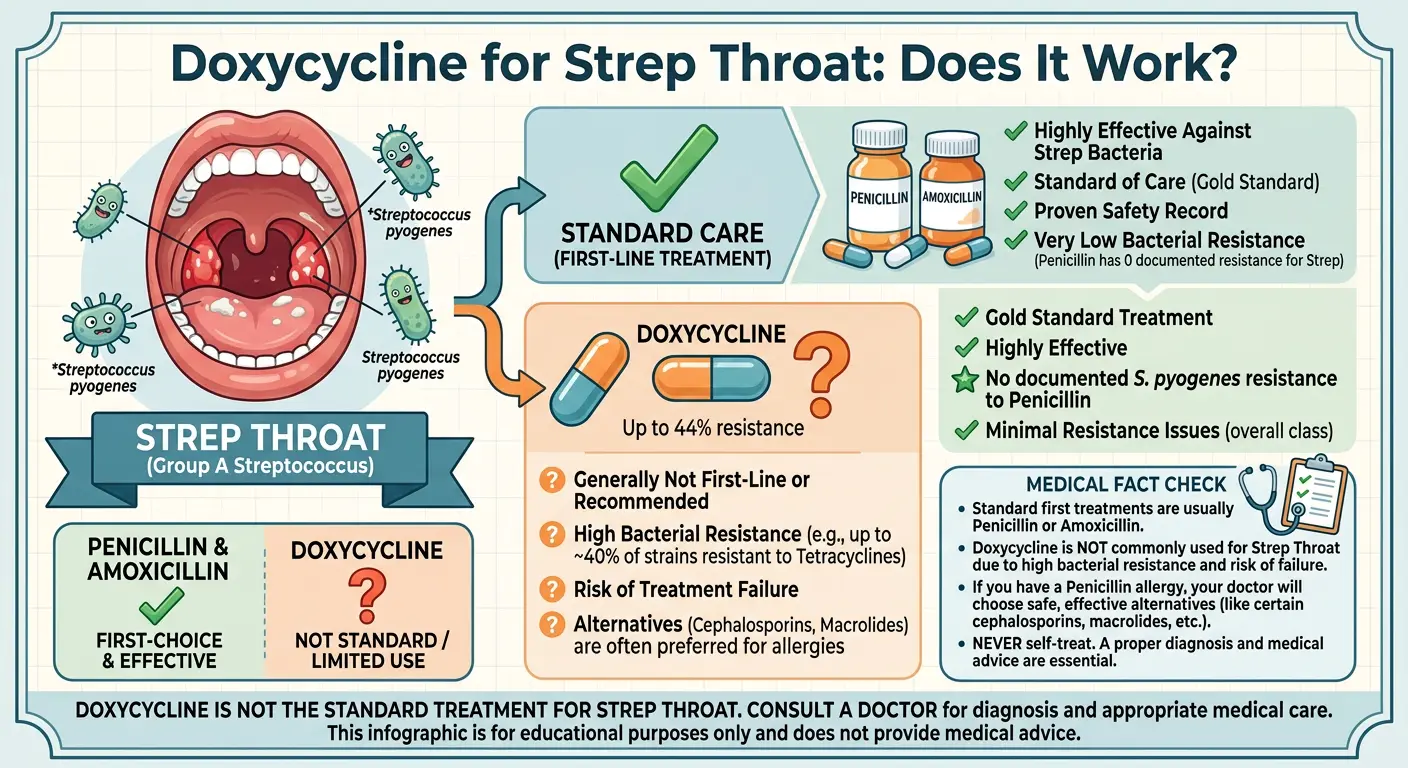
Doxycycline is generally not recommended for strep throat. Due to resistance rates as high as 23.8–39.7% in Streptococcus pyogenes — the bacteria that causes strep throat — doxycycline is considered a poor and unreliable treatment choice. Penicillin and amoxicillin remain the gold-standard first-line treatments recommended by major infectious disease guidelines.
What Is Strep Throat and What Causes It?
Strep throat is a bacterial infection caused by Group A Streptococcus (GAS) — scientifically known as Streptococcus pyogenes. It is one of the most common bacterial throat infections, particularly in school-aged children, though adults are equally susceptible.
Typical symptoms of strep throat include a sudden and severe sore throat, fever, chills, difficulty swallowing, and swollen lymph nodes in the neck. Unlike a viral sore throat — which tends to come with a runny nose, cough, and hoarseness — strep throat is caused entirely by bacteria and, in specific cases, requires antibiotic treatment.
It is worth noting that not every sore throat needs antibiotics. The vast majority of sore throats are caused by viruses, not bacteria. Even when GAS is confirmed as the cause, the infection often resolves on its own. Antibiotic treatment is primarily recommended for patients who have confirmed GAS infection and are at risk of developing serious complications like rheumatic fever or post-streptococcal glomerulonephritis.
Can Doxycycline Treat Strep Throat?
This is one of the most commonly searched questions — and the short answer is: not effectively, and not safely in most cases.
Doxycycline is a broad-spectrum tetracycline antibiotic with activity against a wide range of Gram-positive and Gram-negative bacteria. However, Streptococcus pyogenes — the specific bacteria responsible for strep throat — has developed significant resistance to doxycycline, which severely limits its usefulness as a treatment option.
The Resistance Problem
Clinical studies have consistently shown alarming resistance rates of doxycycline against Group A Streptococcus:
- Resistance rates of 23.8% to 39.7% have been documented among Group A streptococcal isolates
- An additional 15.9% of isolates show intermediate susceptibility, meaning the drug may not fully eliminate the infection
- This level of resistance makes doxycycline a highly unreliable choice for empiric therapy — where a doctor prescribes an antibiotic before lab results confirm which drug will work
This resistance is often driven by the tet(M) gene, a genetic element that allows Streptococcus bacteria to pump tetracycline-class antibiotics — including doxycycline — out of their cells before the drug can work.
Poor Bactericidal Activity
Beyond resistance, doxycycline also demonstrates poor bactericidal activity against streptococcal bacteria. In ex-vivo studies, doxycycline failed to achieve bactericidal levels against Streptococcus pneumoniae at any time point following dosing. This means that even when the bacteria are technically “susceptible” on paper, doxycycline may still fail to fully clear the infection in the body.
Not Recognized in Clinical Guidelines
Major infectious disease guidelines — including those from the Infectious Diseases Society of America (IDSA) — do not list doxycycline as a preferred, alternative, or recommended agent for strep throat treatment. Its omission from these guidelines reflects the medical consensus that doxycycline is simply not appropriate for this indication.
Recommended First-Line Treatments for Strep Throat
When strep throat is confirmed or strongly suspected in a patient at risk for rheumatic fever, the following evidence-based antibiotic treatments are recommended:
First-Line Antibiotics (IDSA Guidelines)
Penicillin V (PEN-VK) is the gold standard for strep throat treatment. It has been used safely and effectively for decades, has an excellent safety record, and Group A Streptococcus has never developed clinically significant resistance to penicillin.
Amoxicillin (Amoxil, Trimox, Moxatag) is equally effective and is often preferred — especially in children — because it tastes better and is available in a once-daily dosing option, which improves adherence.
Penicillin G benzathine is an injectable form of penicillin given as a single intramuscular dose. It is particularly useful in patients where oral compliance is a concern.
For Penicillin-Allergic Patients (Non-Severe Allergy)
Patients with a non-severe penicillin allergy — meaning no history of anaphylaxis or serious allergic reaction — can safely use first-generation cephalosporins:
- Cephalexin (Keflex, Biocef)
- Cefadroxil (Duricef)
These agents have excellent activity against Group A Streptococcus and are well tolerated by most patients.
For Penicillin-Allergic Patients (Severe Allergy)
In patients with a documented severe penicillin allergy — such as anaphylaxis, angioedema, or Stevens-Johnson syndrome — macrolides and related antibiotics are the safest alternatives:
- Clindamycin (Cleocin)
- Clarithromycin (Biaxin)
- Azithromycin (Zithromax)
- Erythromycin (E.E.S. granules)
It is important to note that macrolide resistance in Group A Streptococcus does exist in some regions, so local resistance patterns should be considered when choosing between these options.
When Could Doxycycline Ever Be Considered for Strep Throat?
Given everything above, there are only very narrow and specific circumstances where a clinician might consider doxycycline for a strep-related infection:
- When all first-line agents cannot be used due to documented allergies or contraindications to penicillins, cephalosporins, and macrolides
- When laboratory susceptibility testing has confirmed that the patient’s specific strain of Group A Streptococcus is sensitive to doxycycline
- As part of combination therapy for a complex, mixed infection where doxycycline is targeting a co-infecting organism rather than the streptococcus itself
Even in these situations, using doxycycline would be an off-label, last-resort decision made by a physician with full knowledge of the patient’s culture and sensitivity results — never as a routine or empiric choice.
Risks of Using Doxycycline for Strep Throat
Choosing doxycycline when it is not the right antibiotic for the job carries real and serious risks:
Treatment failure is the most immediate concern. With resistance rates approaching 40% in some populations, nearly one in three patients treated with doxycycline for strep throat may see no improvement — or may actually get worse.
Serious complications can arise when strep throat goes untreated or is inadequately treated. These include:
- Peritonsillar abscess — a painful collection of pus near the tonsil
- Rheumatic fever — a serious inflammatory condition that can permanently damage heart valves
- Post-streptococcal glomerulonephritis — kidney inflammation triggered by an immune response to the strep infection
Contribution to antibiotic resistance is a broader concern. Using antibiotics that are poorly active against the target pathogen — such as doxycycline against GAS — creates selective pressure that encourages bacteria to develop even stronger resistance mechanisms over time, making future infections harder to treat for everyone.
Where Doxycycline Does Work for Respiratory Infections
While doxycycline falls short for strep throat specifically, it remains a valuable antibiotic for other respiratory infections, including:
- Mycoplasma pneumoniae infections — doxycycline is considered a first-line treatment
- Community-acquired pneumonia (CAP) in otherwise healthy outpatients without significant comorbidities — doxycycline is an accepted alternative to macrolides
- Chlamydophila pneumoniae infections — doxycycline is listed as an alternative agent in clinical guidelines
So doxycycline absolutely has a place in treating respiratory tract infections — just not strep throat caused by Group A Streptococcus.
FAQs
Can I take doxycycline if I have strep throat?
Doxycycline is not recommended for strep throat because Group A Streptococcus has high resistance rates to it. Taking doxycycline for strep throat risks treatment failure and serious complications. Always consult your doctor for the right antibiotic.
Why is penicillin still the best treatment for strep throat?
Penicillin has been used to treat strep throat for over 70 years and Group A Streptococcus has never developed resistance to it. It remains safe, effective, affordable, and recommended by all major infectious disease guidelines as the gold standard.
What happens if strep throat is left untreated or undertreated?
Untreated or inadequately treated strep throat in high-risk patients can lead to rheumatic fever — which can cause permanent heart valve damage — as well as peritonsillar abscess and post-streptococcal glomerulonephritis. This is why choosing the right antibiotic matters.
Does doxycycline work for sore throats caused by viruses?
No. Doxycycline is an antibiotic and has no effect on viral infections. Since most sore throats are caused by viruses, antibiotics of any kind — including doxycycline — are unnecessary and unhelpful in those cases.
What is the best antibiotic for strep throat in a penicillin-allergic patient?
For a non-severe penicillin allergy, cephalexin (Keflex) or cefadroxil (Duricef) are the preferred options. For a severe penicillin allergy, clindamycin, clarithromycin, azithromycin, or erythromycin are recommended alternatives.
Final Thoughts
Doxycycline is a powerful and versatile antibiotic — but strep throat is simply not the right indication for it. With resistance rates between 23.8% and 39.7% and a lack of reliable bactericidal activity against Streptococcus pyogenes, using doxycycline for strep throat puts patients at real risk of treatment failure and serious complications like rheumatic fever.
Penicillin and amoxicillin remain the safest, most effective, and most evidence-backed treatments for Group A Streptococcal pharyngitis. For patients who cannot take penicillin, cephalosporins and macrolides offer excellent alternatives — and your doctor will choose the right one based on your specific allergy history and local resistance patterns.
If you have been prescribed an antibiotic for a sore throat and are unsure whether it is the right choice, speak to your doctor or pharmacist. And remember — most sore throats are viral and do not require any antibiotic at all. Responsible antibiotic use today protects everyone’s health tomorrow.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a licensed healthcare provider before starting or changing any antibiotic treatment. For more information, visit https://doxycycline.blog/
